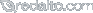Upper Jaw Surgery : Le Fort 1 Maxillary Osteotomy
Upper jaw surgery is technically referred to as “Le fort 1 maxillary osteotomy”.
Why do upper jaw surgery?
The upper jaw can be moved forward to improve the upper lip and midfacial support and correct a negative underbite. The upper jaw can also be impacted or moved upwards to reduce a gummy smile. It can also be rotated to correct asymmetry. The upper jaw can also be impacted at the back to allow the lower jaw to rotate upwards to close an open bite of the front teeth.
How is upper jaw surgery done?
Incisions are made in the gum-line under the upper lip. There are no skin incisions and no facial scarring. The bone in the upper jaw is very thin and can be cut with a micro-saw blade from just under the nose all the way back to behind the last molar teeth. The upper jaw can then be separated and mobilized and moved to the new planned position. The movements have been precisely pre-planned prior to surgery using computerized 3-D software with 3-D printed surgical templates to reproduce the planned movements during surgery. The new position of the upper jaw is fixed using titanium mini-plates and mini-screws. The plates and screws are made from medical grade titanium and are biocompatible so they can stay in place indefinitely. Each plate is precisely bent and shaped to fit over the bone to hold the jaw into the new position. The wires are then released and the jaws are no longer wired together as the plates and screws are now maintaining the new position. Studies have shown titanium to be inert and integrate well with bone. Even though there is no need to wire the teeth together, light dental elastics are placed between the teeth in the immediate post-operative period (usually 4 elastics are used) and patients are later taught to change the elastics daily and these can be removed during eating and cleaning of teeth.
Most patients worry about the pain after surgery however, the pain and discomfort is quite manageable. During surgery, a long-acting local anaesthetic is given so that patients wake up with the local anaesthetic still taking effect and do not initially experience much pain. Patients are connected to a “drip” attached to an automatic pain medication dispenser (“Patient Controlled Analgesia”) which they can activate by pressing a button to provide pain relief. This is removed once patients no longer are using it which is usually in 48 hours after which time oral pain medication is well tolerated.